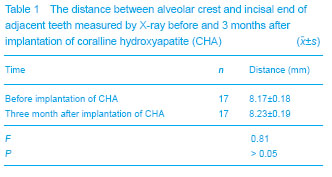
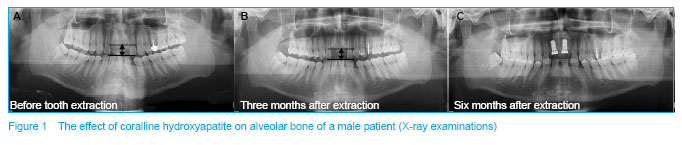
Implant denture can significantly improve masticatory function, similar to the real teeth, especially to solve some complicated cases that normal denture is difficult to solve
[15, 16] . Usually, delayed implant restoration method is to extract teeth that cannot be kept firstly: after its natural healing 3-6 months, dental implantation will be done. However, in the process of self healing of extraction sockets, the alveolar ridge and the surrounding bone have varying degrees of physiologic or pathologic absorption, leading to narrowed alveolar bone thickness and decreased height. Studies have suggested that most loss of alveolar height in anterior tooth area occurs in the first 3 months, and 3-4 mm of the ridge width and height is lost after 6 months
[17] . Adequate alveolar ridge height and width will influence the ideal placement of dental implants and tissue esthetics
[18] .
Socket preservation means to maintain hard and soft tissue after tooth extraction, especially the gingival papilla in the esthetically relevant anterior maxillary area, and a substantial tissue volume is highly critical for the success of implant-retained restorations
[19] .
Recent research has indicated that after tooth extractions there will be physiologic and pathological absorption of alveolar ridge dimensions as a result of normal alveolar bone remodeling. Physical absorption is the oppression of alveolar bone from lip on the organization; pathological absorption is caused by peripheral soft tissue injury in extraction socket and the microenvironment in the progress of natural healing. The contraction of blood clot and accumulation of debris in the tooth socket may limit the potent of alveolar bone regeneration
[20] .
Barrier membrane covering the tooth socket that can reach into the bone maintains a stable environment, in order to reduce the loss of alveolar bone height and width. Animal experiments and clinical studies have shown that filling bone graft materials into the tooth socket can form a bracket, to induce bone formation and reduce the absorption of alveolar bone
[21-23] , which is named membrane guided bone regeneration technology
[24-26] . The membrane prevents the gingival connective tissue and epithelial tissue migrating into the defect and its contained osseous graft, while protecting the blood clots, reduce tissue stress and achieve bone regeneration. The wound stabilization is very important in periodontal repair and may also be of importance for the healing extraction sites.
Autogenous tissue flap and oral biofilm
[27-28] are commonly used as membrane to guide bone regeneration. The use of oral biofilm can always bring about exposure of membrane. However, autogenous free full thickness mucosal flap has been found to be conducive to soft tissue healing and has been reported to serve as a barrier membrane.
The space under membrane determines the size and the morphology of bone regeneration, but only the barrier film itself is unable to sustain the increase of space alveolar bone, and the bone graft material must be depended on
[29] . At present, various bone graft materials existing are widely used in the repair of bone defects. Natural and synthetic graft materials that have been studied in vitro and in vivo and used in different medical procedures in osseous tissue have focused mainly on freeze-dried bone, hydroxyapatite, tricalcium phosphate and coral
[30] . CHA (Tianbo Chigu) is a newly developed artificial bone graft polymer material, which is composed of high quality marine corals, chemical formula is [Ca10(PO4)6(OH)2], the character is the powder granular. The ostiole on skeleton (CaCO
3) of coral hydroxyapatite thin layer provides a good space for the tissue growth. Additionally, CHA contains two hydroxyl groups, which can bond water molecules by hydrogen, so to have a good hydrophilicity. The benefits of CHA as bone graft are predominantly its safety, biocompatibility and osteoconductivity so that it can be used as a substitution biomaterial for bone in many indications clinically.
This study used autogenous free full thickness mucosal flap and CHA (Tianbo Chigu) to restore the shape of alveolar bone
[31-32] . After operation, macroscopic observation and X-ray showed that the loss of height and width of alveolar bone was reduced. In this research, porous maxillary anterior bone was chosen, because the bone has rich blood circulation, sensitive marrow stromal cells and good ability of anti-infection. A good bone graft bed filled with substitute materials after tooth extraction will provide good support conditions for planting denture.
These cases indicated that there were several methods to reduce or avoid bone absorption after teeth extraction: (1) For reducing cicatrix of soft tissue, operator trys to avoid doing any incision on gum; (2) atraumatic extraction can help preserve the residual supporting bone; (3) bone graft materials, such as CHA, are grafted into the socket, and replaced by new bone slowly; (4) mucoperiosteal flap at palatal side covering graft area after tooth extraction cannot only prevent gingival recession because of tissue pulling, but also form good sealing to isolate the accumulation of debris in the tooth socket, and to promote bone regeneration.
Given the vast scientific evidence and documentation of the above information, the benefits of conducting CHA in socket after tooth extraction and covering the wound with mucosa flap is emphasized. It is recommended to use CHA as graft material. CHA improves the prognosis by maintaining the residual bone and realizes the purpose of sockets preservation. Thus, hydroxyapatite as a bone graft material has good bone compatibility and security, which is worthy of development.